

Connect your vendor data on one platform with advanced predictive insights to make smarter benefits decisions, measure the value of your point solution programs, and improve employee health and productivity.
Simplify and accelerate your decision-making with our connected data platform
Partner with a team of highly responsive analytics experts
Have confidence in your ability to improve member health, well-being, and productivity
Choose the right point solution programs and measure results
Unify your data on one platform with predictive insights to uncover new opportunities for cost savings
Improve benefit design and match the right members to the right programs to avoid high-cost outcomes
As a benefits leader, you're investing in point solutions to boost employee health and productivity, but these programs are difficult to track and measure. You want to help your employees and contain costs, but how can you be sure you're achieving these goals?
Gain confidence in your decision-making with easy-to-understand dashboards that put answers at your fingertips and help you build a strong ROI narrative for internal stakeholders.
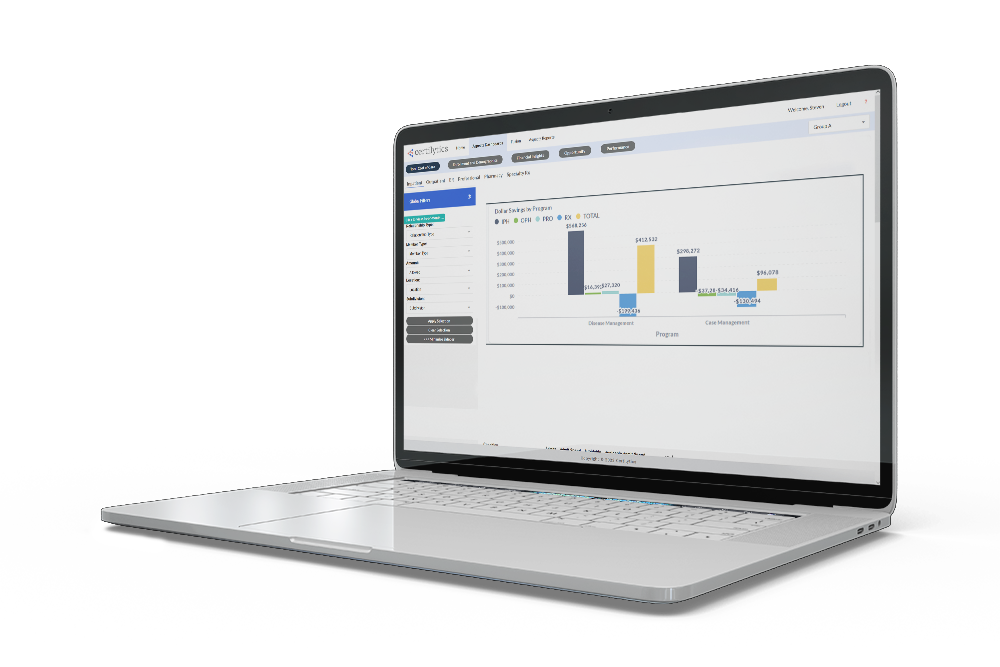
Understand the potential impact of solutions to optimize your strategy
Maximize employee engagement by investing in the right programs
Transparently measure program performance and ensure ROI
Case Study: How to Choose the Right Point Solutions and Measure Results
How one Fortune 100 employer maximized solution impact to achieve over $200 in PMPY savings
Certilytics' predictive insights support health & wellness programs for dozens of large, self-funded employers. A retrospective analysis shows these programs save participating employers an average of over $200 PMPY while improving employee health.

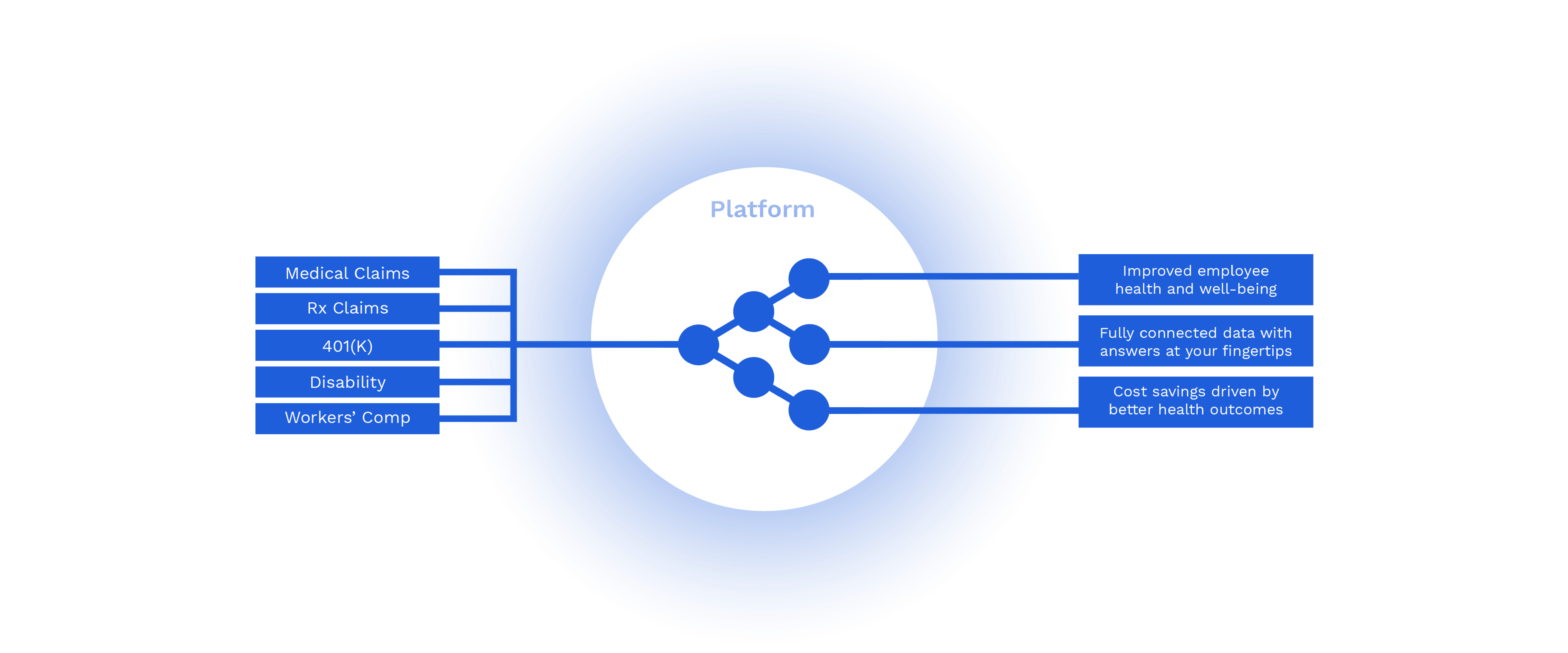
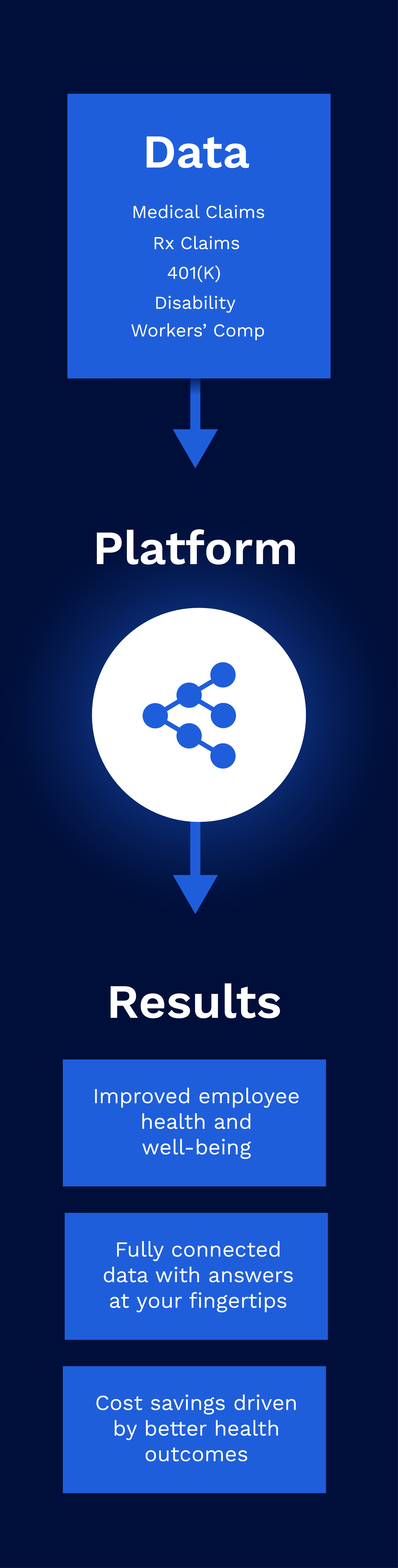
Simplify and accelerate your decision-making with a next-generation data warehouse that transforms your benefits data into actionable intelligence. Improve benefit design, coordinate care across vendors, and incentivize health partners shift from free-for-service to value.
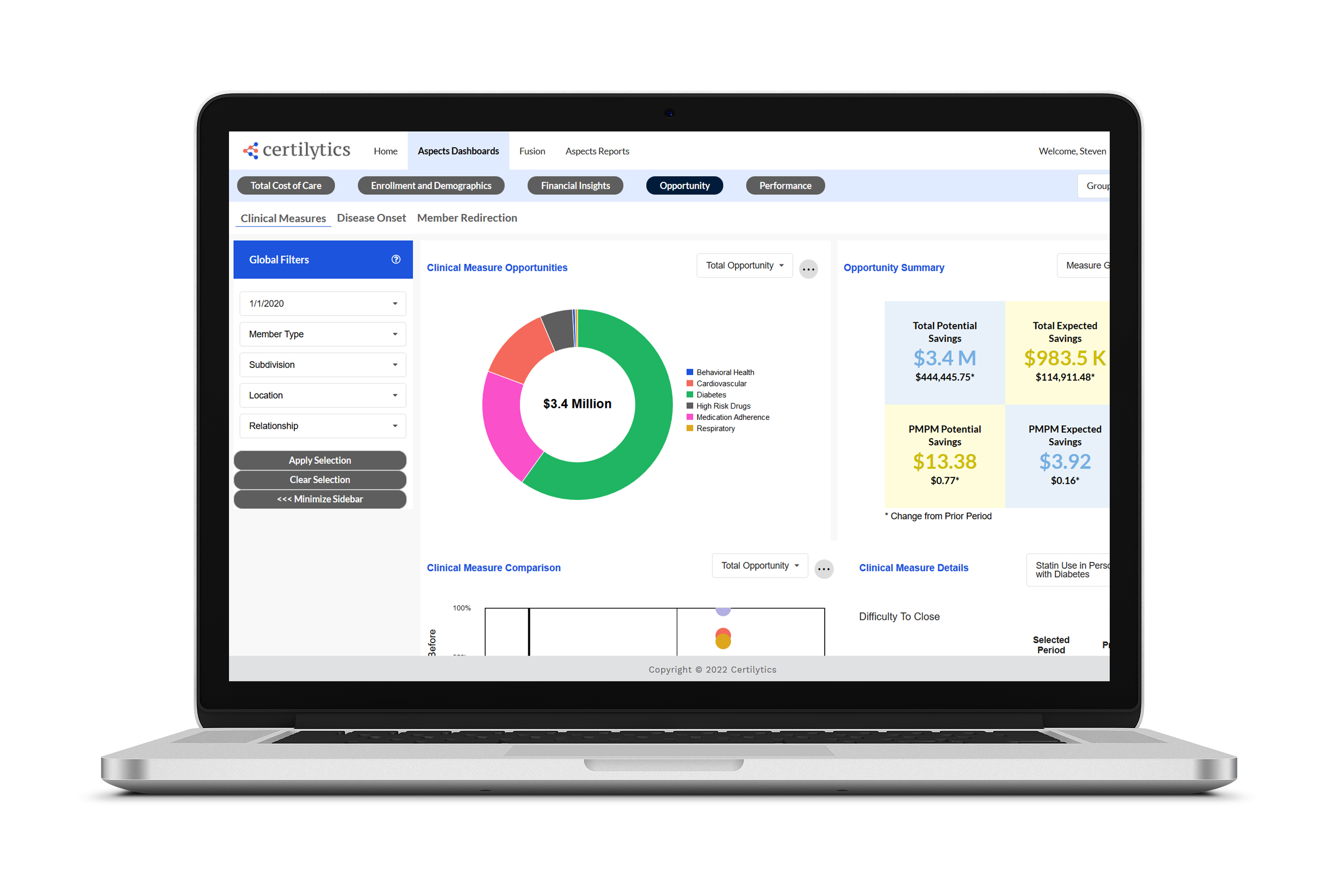
Pre-built dashboards and self-service analytics at your fingertips
loading..
What Sets
Certilytics Apart
Whether you're looking for high-level population trends or in-depth analyses, our easy-to-understand dashboards and self-serve data exploration tools will simplify and accelerate your decision-making
Unify all your benefits data on one modern, flexible platform that gives you a comprehensive view of your population with click-through capabilities down to the member or claim-line level
We process 30M+ member lives per week to ensure our customers have the real-time insights they need to make smarter decisions, faster
We keep you at the forefront of proactive, AI-powered decision-making through an iterative approach to product design and innovation
You'll love working with our team of experts to connect and understand your benefits data. We are committed to answering your questions, getting you up to speed on our reports and dashboards, helping you transform the way you do business, and ensuring you get real value from our solutions
Our reporting looks forward, not backward, with market-leading predictive models that show you not just what's driving cost-but what's driving avoidable cost
Schedule a 15-minute introduction call, 30-minute overview of our solutions or a 90-minute demo