Diabetes affects about 10% of the U.S. population and accounts for hundreds of billions in annual healthcare spending and lost productivity, according to the CDC and American Diabetes Association.
For our customers, the financial impact is significant. Diabetes care accounts for 3-5% of their total healthcare spend, with common medications such as Trulicity, Januvia, and Jardiance costing between $550 and $775 for each refill and tens of thousands of dollars annually.

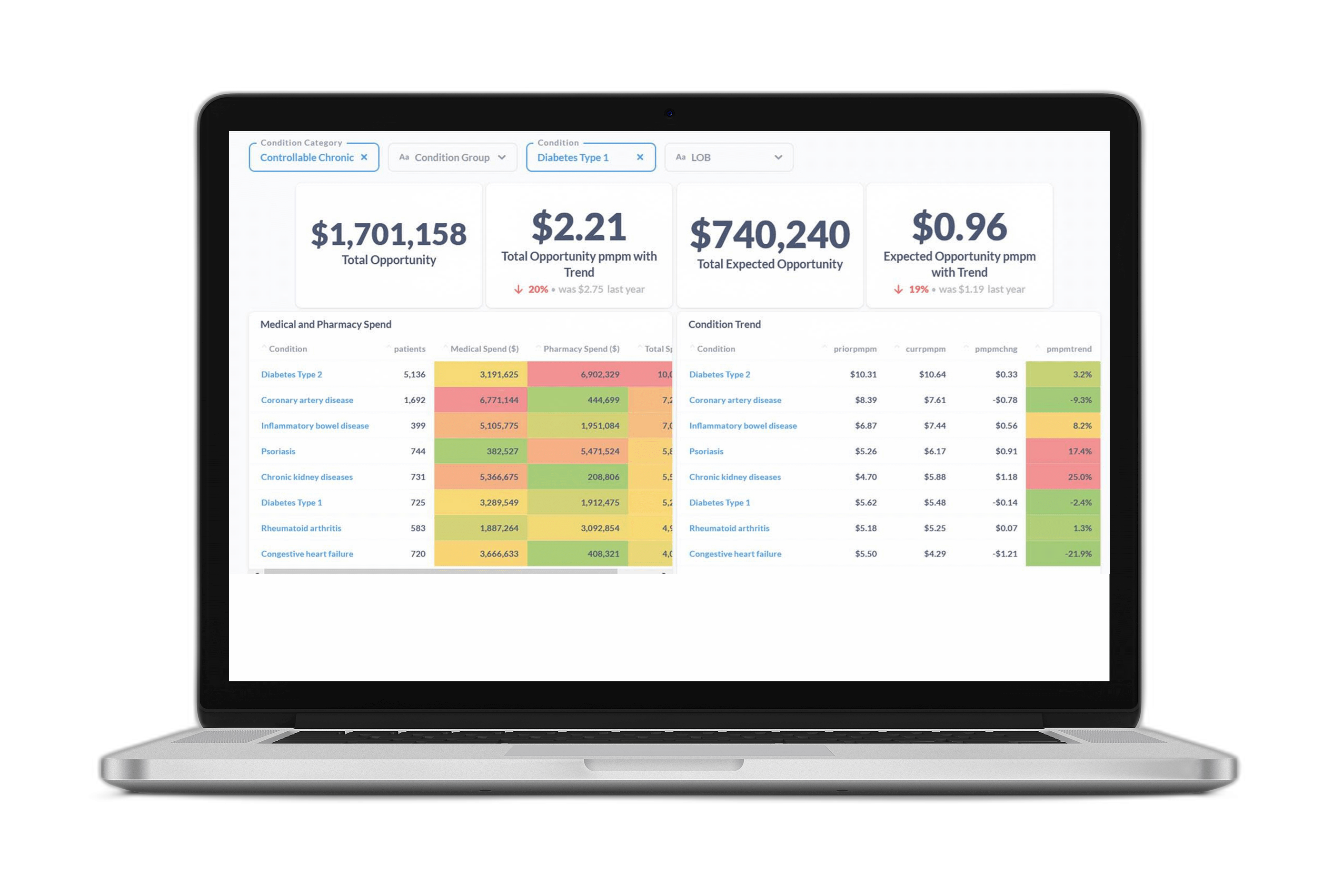
We’re working with some of the nation’s largest health plans, provider health systems, and self-insured employers to reduce these costs while improving member health and well-being. By applying AI-powered insights to their diabetes and drug management programs, we’re able to boost the effectiveness of these strategies and enable more targeted interventions.
Removing Uncertainty from Diagnosis & Treatment
Certilytics’ models have market-leading predictive accuracy, enabling our customers to determine which members are most at risk for diabetes and understand the outreach methods that would be most effective at preventing or better managing the disease.
In addition, our customers use our predictive intelligence to measure the effectiveness of their clinical point solutions—enabling them to determine which diabetes management programs best serve the needs of their population.
Diabetes is often accompanied by other comorbid conditions, and, depending on a person’s lifestyle and health history, different factors can play into a diabetes diagnosis. An effective treatment pathway for one member may not be effective for another.
With our data warehousing and predictive analytics platform, our customers develop personalized care delivery strategies to ensure that members are matched with the right care pathways and clinical point solutions at the right time.
With this insight, diabetes management no longer has to feel like trial and error. Payers and providers can see risk on the horizon, align clinical and financial strategies, measure impact, and transparently communicate the value added to clients and their consultants.
Ready to see how it works? Meet with our experts!