We were thrilled to make new connections and see familiar faces at the IBI/Conference Board Health and Productivity Forum.
From the solution showcase and cocktail reception to the conversations at our exhibit, we were grateful to those who took the time to connect with our healthcare and predictive analytics experts.
Check out 3 topics dominating our discussions with benefit leaders while in Chicago.
Topic #1: Selecting the Right Digital Health Solution
With the pressure to contain costs and improve employee well-being, benefit leaders have turned to digital health solutions to improve their benefit offerings.
Many employers are managing or considering multiple solutions at once. With so many options available, it makes sense that many employers are overwhelmed – from disease management programs to digital wellness apps to fitness trackers and more.
They want more confidence that they selected the right solution, and will be able to evaluate that solution effectively once they’ve chosen it.
Data and analytic platforms have the ability to integrate the data from all these vendors into one source of truth.
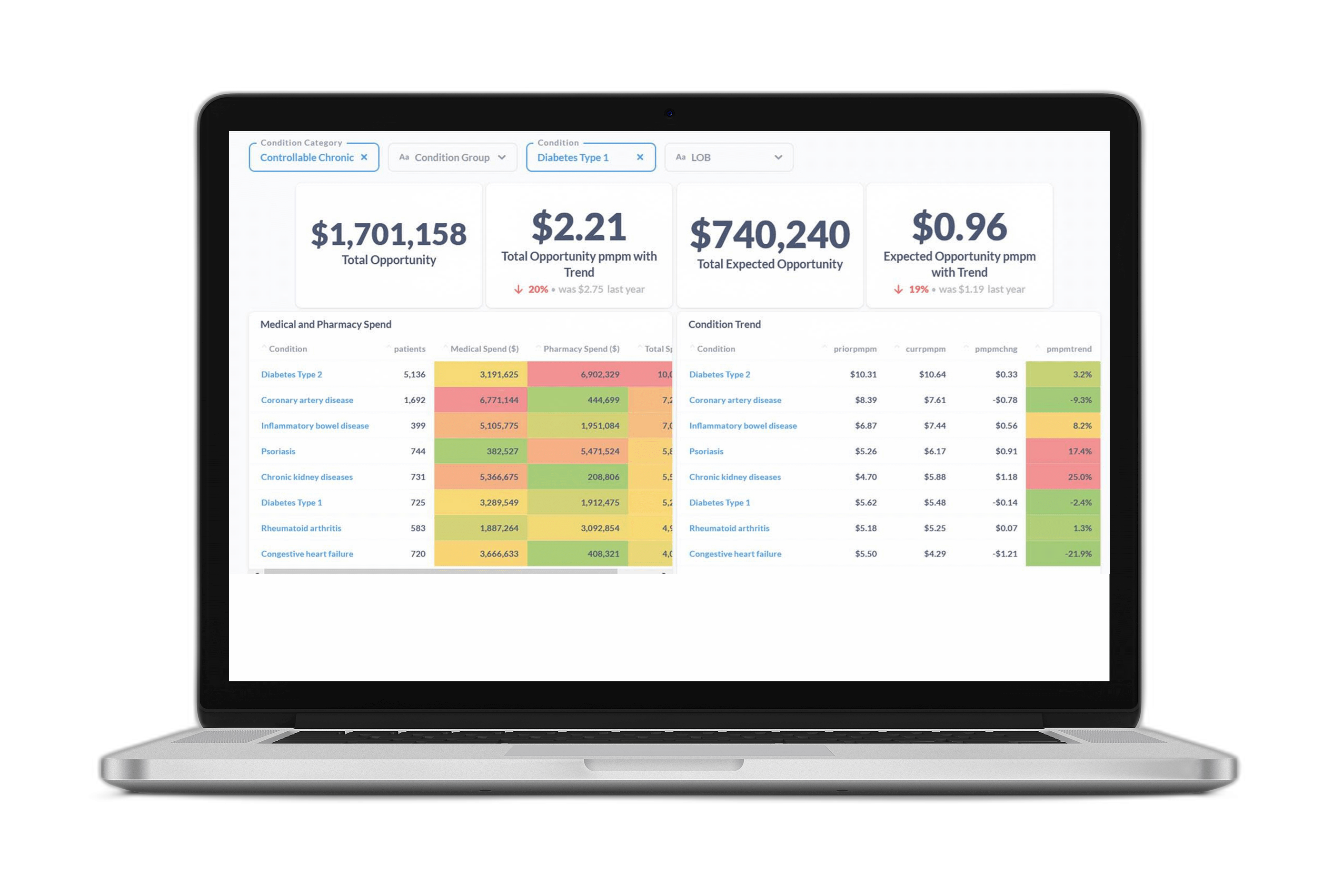
Many benefit leaders at the conference are starting to turn to AI-powered tools like Certilytics’ Program Performance Analytics solution to help measure performance, ensuring employers that performance guarantees are being met, programs are being utilized, and costs are reducing.
Topic #2: Shifting from Reactive to Proactive Benefit Strategy
Most benefit leaders talked about how they have been used to pursuing the best discounts and widest networks with health plan partners, but now are working toward a more holistic benefit strategy – one that prevents rather than reacts to high-cost events.
In order to better anticipate unique employee needs, more employers are shifting to AI-based analytic tools.
The capabilities of tools like Certilytics’ AI-powered platform gives benefit leaders a holistic view of their employees’ health, enriched with predictive insights.
With these insights, benefit leaders can visualize the future prevalence of specific conditions and the avoidable costs on the horizon, plus test potential programs as well as point solution vendors to see which will have the biggest impact on health and costs.
Topic #3: Closing Health Equity Gaps and Addressing Mental Health Challenges
Employers are facing new expectations from employees.
Increases in mental health needs have helped drive efforts for more holistic benefit strategy that both addresses social barriers to preventative care and provides wrap-around proactive benefits for employees.
Predictive and data analytic platforms are helping address these changing expectations. By unifying and adding predictive power to their data, employers can locate pockets of risk, understand under-utilization of programs, and pinpoint which programs, solutions, or resources would have the greatest impact.
Thanks again to all those who made time to connect with us in Chicago—we hope to connect again (or for the first time) at next year’s conference!
To learn more about Certilytics AI-driven predictive analytic solutions for benefit leaders, schedule a meeting with our team.