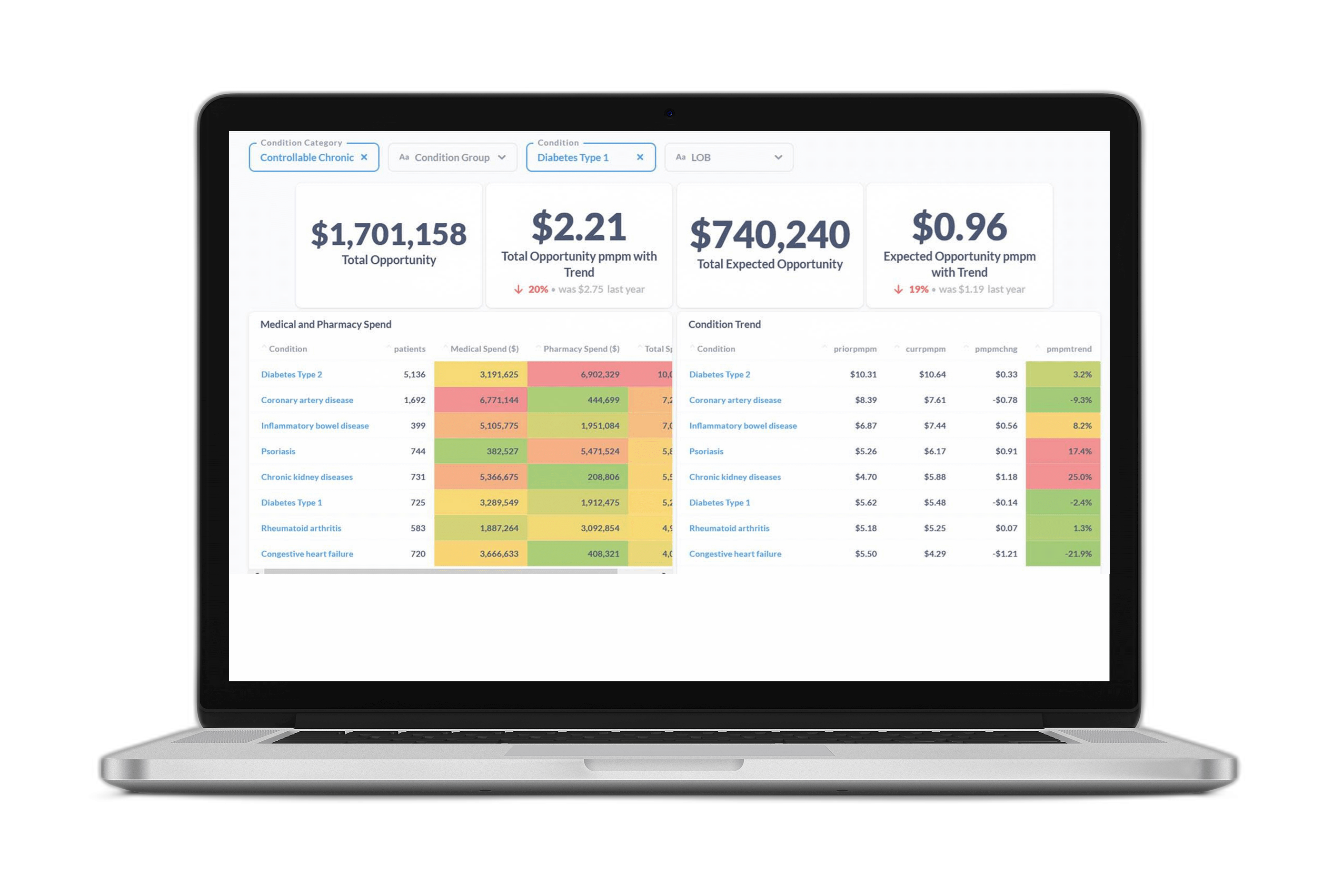
Chronic diseases carry significant health and cost impacts for healthcare payers, and this reality became even starker during the pandemic.
Conditions such as obesity and heart disease can cause more severe COVID-19 symptoms, according to the Centers for Disease Control and Prevention, exacerbating the health and economic toll both these diseases have on healthcare payers and providers alike.
Obesity affects 20% of children and 42% of adults, putting them at risk of chronic diseases such as type 2 diabetes, heart disease, and some cancers. Obesity also comes with a nearly $147 billion a year price.
Heart disease is even deadlier, with more than 877,500 heart disease or stroke deaths in the U.S. each year, the CDC notes. It also costs the health system $216 billion per year and $147 billion in lost productivity.
Healthcare payers are increasingly turning to predictive models to enact proactive strategies that direct care management resources to those who will benefit most–improving health outcomes and reducing costs.
Here are the top three predictive models healthcare organizations can use for heart disease and obesity prevention:
1. Heart Disease Model
Every 40 seconds, someone in the United States has a heart attack, according to the CDC.
Predictive insights are crucial to detecting those at risk for heart attacks before a hospitalization or even death occurs. Earlier interventions driven by forward-looking insights can also help prevent the onset of other associated conditions.
With this deeper understanding of emerging risk and its main drivers, healthcare payers can shift to preventative strategies including proactive, personalized engagement and education strategies.
2. Hospital Readmission Risk
Obesity increases the burden on hospitals by not only driving up the number of avoidable hospital visits but also lengthening the duration of hospital stays, studies have noted.
Predictive insights are critical to helping healthcare organizations break the cycle of repeat hospital visits by shedding light on when a discharge is appropriate and identifying complications such as obesity and heart disease that are driving the repeat visits.
Rather than treating complications that stem from checking out a patient too early, payers and providers armed with predictive insights are able to coordinate effective discharge planning from the time a patient checks into the hospital.
This ensures that the patient’s needs are met throughout the care continuum, helps reduce avoidable overspend, and addresses underlying causes for a hospital visit before a patient is readmitted.
3. SDOH Model
Gaining a clear picture of the impact of heart disease and obesity on a population through a health equity lens is essential for impactful preventative strategies that improve access to care.
Social Determinants of Health (SDoH)-focused predictive models provide insights into which segments of the population should be prioritized for an intervention, pinpointing the geographic area where investment and resources would be best allocated.
Effective SDoH predictive models also give healthcare leaders the ability to test hypotheses prior to implementing new programs to ensure they are creating real value. They can prioritize outreach initiatives such as educational programs, placement of new clinics, or targeted telehealth outreach.
Did You Know?
- Certilytics’ “Hospital Readmission Risk” model leverages deep learning to predict a readmission within 30 days of discharge after an acute hospitalization.
- Certilytics’ “Heart Disease Model” calculates the risk that a member will suffer a heart attack within the next 12 months.
- Certilytics’ “SDOH Model” quantifies and predicts SDoH-derived risk. Our model answers not just the “who” and “where” of SDoH risk, but the “why” and “how.”
For a free consultation with our team of experts on how you can leverage predictive insights to transform your organization, reach out to us at contact@certilytics.com.