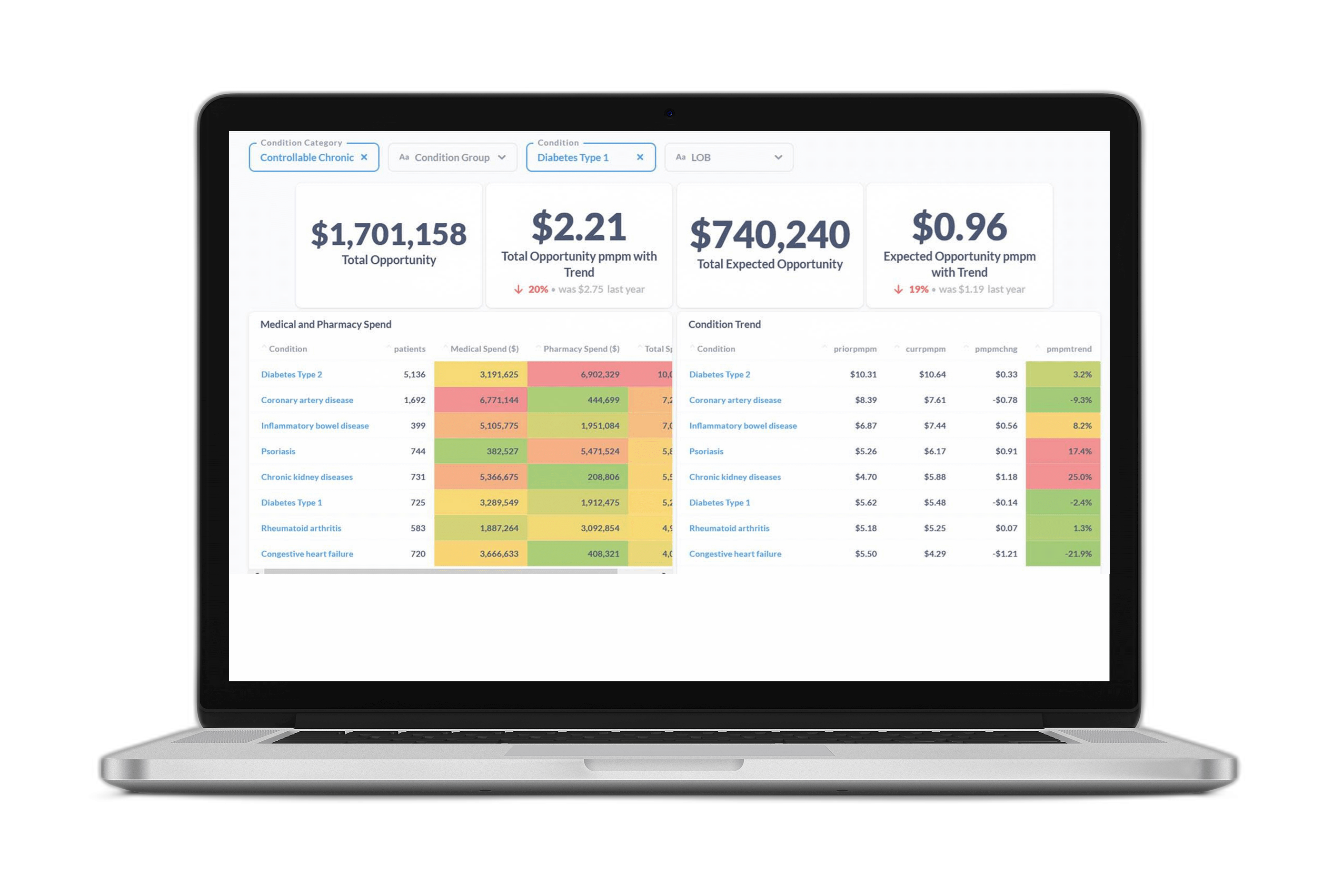
“Social Determinants of Health.” It’s long been a major topic of conversation among healthcare leaders, but COVID-19 has increased the urgency to translate the concept into practical, real-world solutions.
The pandemic has deepened awareness about the disparities in medical and behavioral care access caused by factors such as income, food deserts, education, and housing stability. At the same time, national conversations about inequality have caused employers to reexamine their benefit plans while health plans and provider health systems are implementing personalized care strategies.
But if there’s anything clear about social determinants of health, it’s that there’s no standard manual for measuring and addressing them. There’s a lack of consensus about the care strategies and treatment pathways that will effectively close care gaps and respond to these various social inequities that have a major impact on health outcomes.
Payers face an array of challenges from identifying the specific social health barriers faced by their target populations to accurately measuring the outcomes of interventions.
These challenges have driven many of the nation’s largest healthcare organizations to replace their standard reporting capabilities with advanced predictive analytic and data warehousing tools that can better predict and quantify SDoH risk.
Still, finding the right data partner brings its own set of challenges. Whether you’re looking to replace your existing technology or just starting your search for a new tool, there are some essential things to look for in a data partner.
Below are three questions you should ask when selecting a data partner to help you build a successful SDoH strategy:
1. Can your partner connect all your data for a 360-degree view of patient health and well-being?
In general, there can be broad signs that social health barriers are impacting the health of your population. There may be an uptick in absenteeism, higher instances of emergency room visits, lower medication adherence, or signals of lost productivity.
But understanding at an individual level which social factors could be driving these issues – and how and why – is key to knowing which combination of interventions will address them most effectively.
Data gaps make it notoriously difficult to find these answers. There is typically more than one SDoH factor at work within a population, and the signs of these barriers can be dispersed across many data feeds.
Standard analytic tools that look backward often leave health plans and benefit teams reconciling multiple reports to connect the dots—leading to reactive strategies that miss opportunities to proactively drive engagement.
In addition, employee turnover has only increased during the pandemic, giving benefit teams an influx of new employees for whom there’s limited historical healthcare and benefits data.
The right data partner will be able to aggregate data from across the care continuum to provide a 360-degree view of each member’s health. For example, Certilytics’ AI-powered SDoH model uses mix of zip code and household-level SDoH data—in addition to medical and pharmacy claims and dozens of other data sources—to give payers an understanding of the SDoH factors negatively impacting health outcomes as well as an understanding of those patients most likely to engage with outreach.
Our model doesn’t just answer the “who” and the “where” of SDoH risk, but also the “why” and the “how.” Why is a given patient high risk? What strategies and interventions would most effectively reduce that risk? With these insights, payers can prioritize patients for outreach and deploy non-clinical resources that have the greatest impact on cost and health outcomes.
If a vendor isn’t providing this holistic view of population health, particularly cross-benefit analysis across pharmacy and medical records, then it may be worth shopping for a new tool.
2. Do your analytic tools help you measure the value of existing and potential partnerships?
Researchers have pointed out that one of the biggest challenges for implementing a successful SDoH strategy is developing effective partnerships with community-based organizations.
While the number of such partnerships has increased in recent years, payers have struggled to handle the capacity challenges of these organizations, which often lack sufficient resourcing and infrastructure. It is usually left to health plans or self-insured employers to define the value-based goals of an intervention, the metrics of success, and the payment model structures.
Using our SDoH predictive model, healthcare leaders can test hypotheses prior to implementing new programs to better understand the business case for a partnership and quantify the potential value. Equipped with AI-powered reporting, payers can prioritize outreach initiatives such as educational programs, the placement of new clinics, or targeted telehealth outreach.
This enables payers to start a conversation with a community partner with a clearly defined scope, goals, and success metrics.
3. Does your partner measure the success of your interventions?
The increases in investments in SDoH solutions and partnerships has made evaluating the performance of these investments even more critical. Yet many payers implementing these programs and partnerships are left with more questions than answers. Did medication adherence improve as a result? Which care gaps were closed, and why? What’s the value, in dollars, of each partnership and program?
Benefit and health plan teams need real-time updates to see if their investments were worthwhile. An effective data partner gives health plans and benefit teams the ability to see SDoH risk at both a patient and population level, enabling payers to regularly track the progress and value of their programs.
If you’re interested in learning more, contact us for a free consultation with our team of experts or check out our innovative AI model that predicts and quantifies SDoH-related risk.