We were thrilled to make new connections and see familiar faces at the HIMSS 2023 conference.
Our team had a lot of inspiring and thought-provoking conversations with fellow attendees, and we thank those who took the time to connect with our healthcare and predictive analytics experts.
Whether it was during a shuttle ride, waiting in long lines for coffee, during the debut of our Price Transparency Analytics solution to live demos at our booth, all our conversations made clear that healthcare leaders are looking for innovative, data-centered approaches in order to tackle healthcare’s biggest challenges.
Here are the top 4 hot topics our conversations centered around at HIMSS this year:
Topic #1: Shifting to Value-Based Care Strategies
Health plans, plan sponsors, and provider health systems all shared their focus on developing strategies that will help their organizations shift to value-based care.
In sessions, forums, and at our booth, the predominant questions from healthcare leaders were how can I use my data to:
- Identify the most effective ways to improve health outcomes?
- Develop whole-person strategies that also reduce my healthcare costs?
- Measure the success of the programs and strategies I implement to support our value-based care goals?
Traditionally, leaders have relied on retrospective risk analysis and utilization rates when deciding who to target with programs and where to allocate their resources. But this analysis was built to serve the fee-for-service model, not achieve value-based care goals.
To answer these questions, healthcare leaders need to leverage the mountains of data at their disposal. More than just allowing a data partner to connect all these disparate data sets, these leaders need a partner that can enrich their data with predictive analytics.
Meeting value-based goals depends on how successful you are at unlocking the value in your data. At Certilytics, we believe unified data and smarter analytics is key to driving more efficient and affordable healthcare.
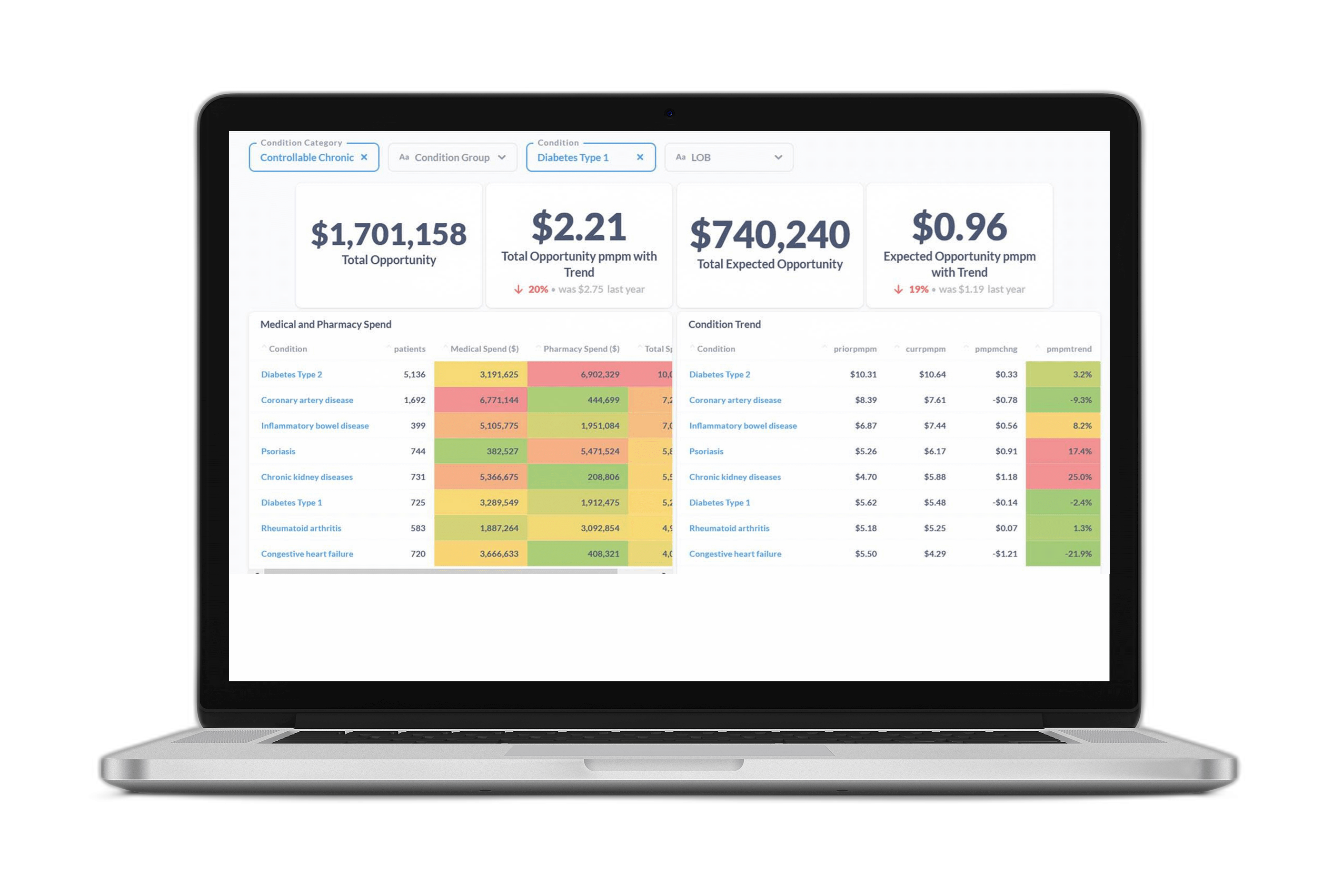
Across our solutions we provide our customers with an Opportunity Analysis that identifies a member’s future risk for being diagnosed with a condition or experiencing a high cost event, including the associated financial costs. This helps our customers identify where to invest in building programs and strategies that will help reduce costs while also improving the health of their population.
Topic #2: Assessing Risk within a Population is a Building Block of Value-Based Strategies
As one healthcare leader who visited our booth put it: “Succeeding in value-based care starts with identifying those who are at risk. If you know who is at risk, you can build support and strategies to keep them healthier.”
Healthcare organizations are taking it even a step further by wanting to not just identify risk in their population, but how to direct their resources to the member or employee who will benefit most.
Traditional data analysis ignores the fact that the highest-cost members aren’t always the ones who will modify their behavior or benefit most from clinical intervention. A member with lower overall predicted financial risk—but more open care gaps—might be a better candidate for outreach, especially if the member shows a high propensity for engagement.
It’s why those who saw our predictive analytics platform in action at HIMSS were excited to see our insights taking into account not just a person’s risk, but also their willingness to engage with outreach. This intelligence will enable them to target the right member with the right programs at the right time.
Topic #3: Price Transparency Data has the Power to Disrupt Healthcare
Everyone wants to know how to turn this new access to healthcare data into valuable intelligence, but the data sets themselves are anything but transparent.
So, health plan leaders are looking for solutions that will unpack these large, complex MRF files so they can see exactly where they stand relative to other health plans.
For example, at our HIMSS presentation, healthcare leaders shared with us their excitement about our new Price Transparency Analytics solution and how it will give them the kind of easy-to-understand intelligence they need to remain competitive.
Takeaway #4: Large Language Processing is Opening up New Possibilities in the Healthcare Space
One keynote panel speaker put it succinctly: “The opening of the ChatGPT service launched AI into the public consciousness, and it has made a daily appearance in the news ever since.”
ChatGPT and other larger language processing models have put a spotlight on the use of advanced machine learning concepts to search, analyze, organize, and interpret large amounts of data in the healthcare space.
This has a number of applications, both at the point of care and for payers looking to leverage new predictive insights to drive down costs.
Thanks again to all those who connected with us in Chicago! If you’d like to schedule time with our team to keep the conversation going, book your meeting today.