With the passing of the Consolidated Appropriations Act of 2021, employers like you were given a lot more responsibility over the healthcare services you purchase for your employees and their families.
While these regulations made headlines, not much has been said on how exactly you can be sure you’re serving as the best steward of your health and benefit offerings.
So, how can you be confident your healthcare services are as efficient and affordable as they can be? What does success in this role look like?
The good news is we can help you. We’re partnering with self-funded employers to find these answers in their data so they can quickly and effectively adopt strategies that enable them not to just comply with the regulations, but turn this responsibility into an opportunity to better meet the needs of their employees and their families.
Here are three essential things employers must have from their data and analytics partners in order to turn compliance into opportunity:
1. Find a Data Partner to Help Unify and Enrich Your Data with Predictive Analytics
To ensure the benefit decisions you are making are in the best interest of your employees, you must first understand their existing and emerging needs.
This understanding begins with a complete picture of your employees’ and their families’ overall health.
This can certainly be a challenge given all of the data from your health partners and program solution vendors. Especially since most employers haven’t traditionally been in the business of collecting data beyond medical and pharmacy claims.
So what’s the best way to connect your data?
This is where a data partner comes in. You’ll need your partner to not only collect your data from all these different sources, but link it all together.
By doing this, you can be confident that your benefit decisions have come from a single, precise source of truth.
How can predictive analytics be a game-changer?
Connected data will help you meet your fiduciary responsibilities, but enhancing your data with predictive analytics will help you succeed. If your data only tells you what has happened in the past, you can’t make the best decisions for your health benefits plan now and in the future.
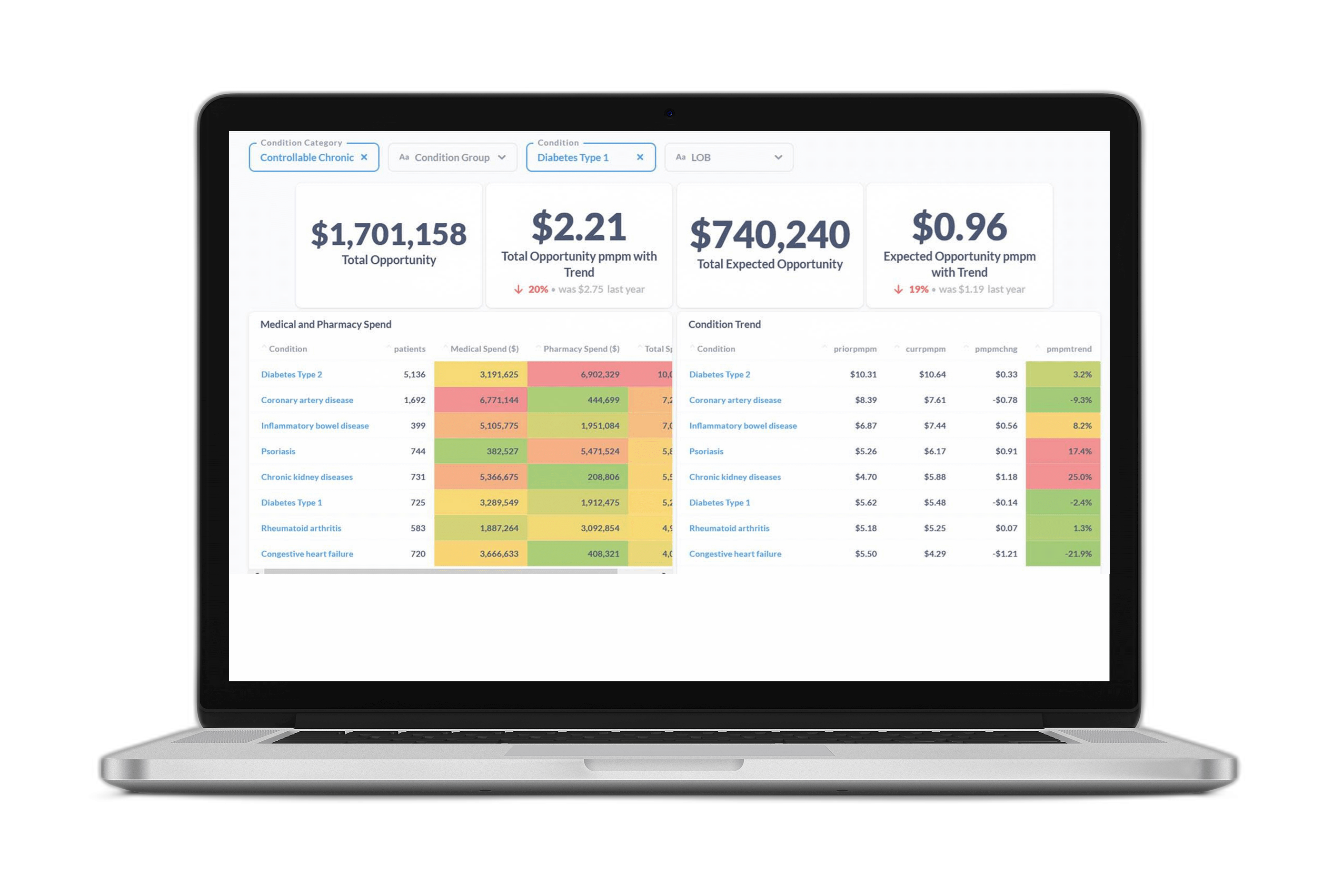
A predictive analytics partner enables you to look forward and identify emerging trends and health risks within your employee population. For example, below is a snap shot of what our customers see when they leverage our predictive analytics solutions. They can identify the highest areas of spend, which is the first step in implementing programs and strategies to proactively minimize those costs and keep their employees healthier.
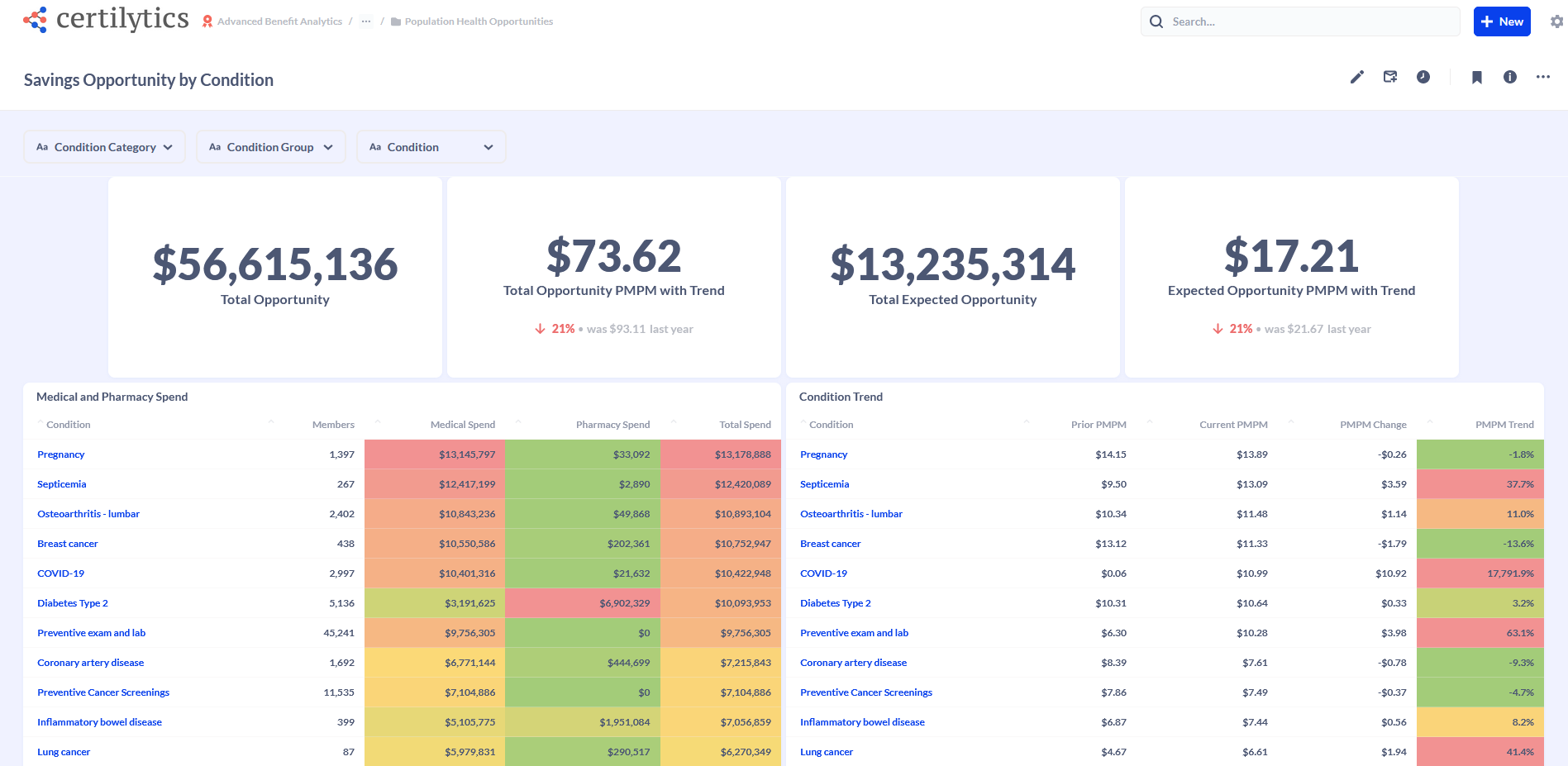
2. Use Your Data to Identify the Largest Opportunities for Cost Savings and Improved Health Outcomes
Once your team understands the risks and needs in your population, you can begin exploring the most effective ways to keep your employees and their families healthy.
The key is knowing the best ways to reach them. This insight is the difference between just identifying risk and actually improving health outcomes. It’s also integral to not just pinpointing high costs, but addressing avoidable spending.
How do you know who will respond to point solution vendors’ efforts? How do you know which type of outreach methods would generate the most engagement?
A predictive analytics partner should answer these questions for you, allowing you to build proactive programs around these individuals.
For example, at Certilytics, we provide our customers with an “Expected Opportunity” score. It is this opportunity that accounts for the likelihood of an employee to engage and change their behavior. With our platform, you can see the likelihood of engagement down to the individual level, enabling you to build programs that match the right employee to the right program at the right time.
3. Leverage Your Vendor Partners’ Data to Evaluate the Impact of Programs and Strategies on Reducing the Total Cost of Care
Your data has helped you build programs that will have the greatest impact on health outcomes and costs.
But, how can you be confident you made the right decisions?
You need a data partner who can work with you to collect data from all your solution vendors and evaluate their performance from both a health and cost perspective.
At Certilytics, our predictive insights are helping our customers track the progress of their point solution programs and measure their impact on ROI. With this insight, they assess which programs are most effective at impacting behavior, improving health, and reducing healthcare costs.
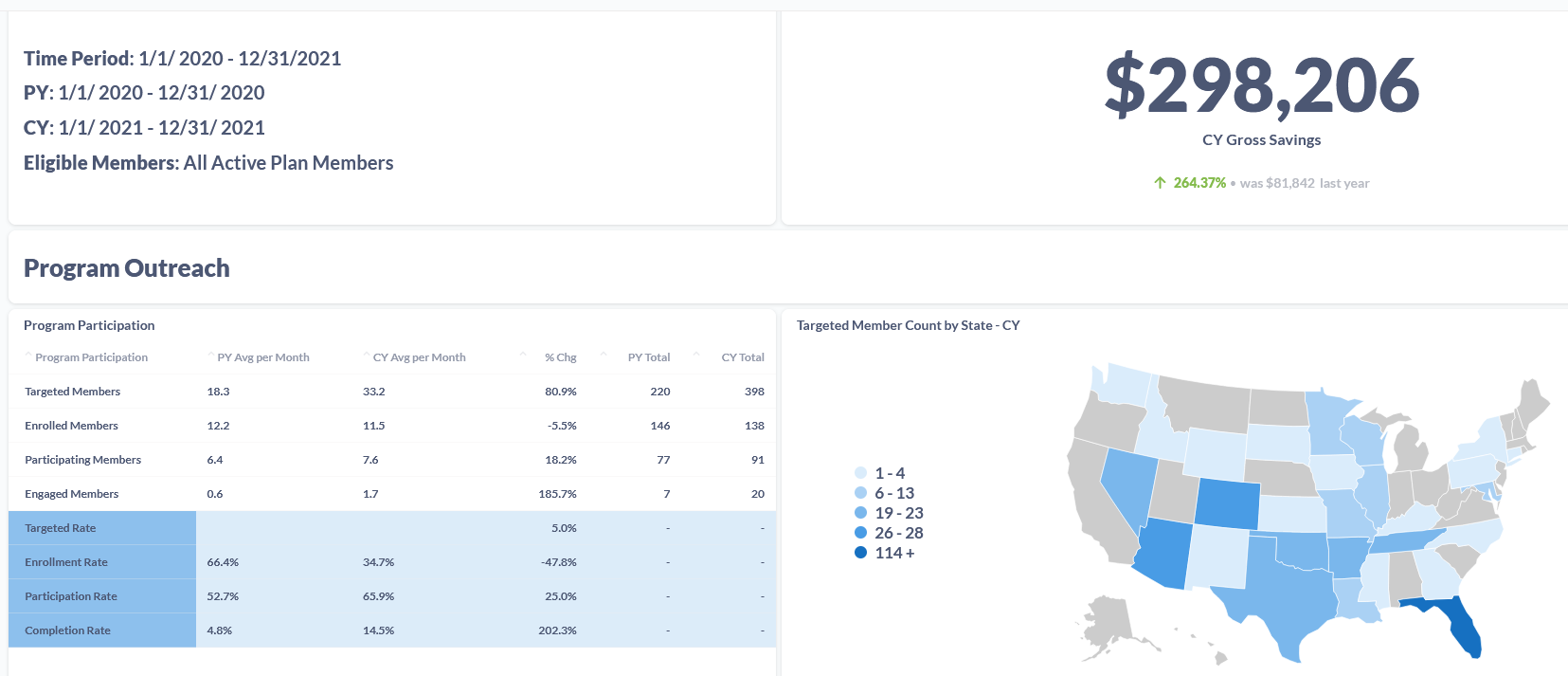
Want to learn more about how Certilytics can help you leverage your data to succeed in your role as a fiduciary of your health plan?